Be in the Know with Your Pro
As a registered dietitian and board-certified specialist in sports dietetics, I am all about communicating the importance of consistency, quality and quantity of foods to eat to strategize, optimize and realize goals. To be strong, go long, restore to do more… it is important to get the most out of food choices. With many of my athletes/active clients expressing interest in plant-based eating, I want them to capitalize on food choices to maximize the benefits. So how can you be plant-based and still meet your nutrient needs to support fueling for exercise and recovery?
Consider soy foods, which were highlighted in the 2020-2025 Dietary Guidelines for Americans as great food choices in the protein category and the only plant based nutritionally appropriate alternatives for milk and yogurt. (U.S. Department of Agriculture and U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 2020-2025.
Why do food choices matter to active individuals?
Optimizing intake is not only beneficial for performance but also health. Carbohydrate and fat are critically important as fuel sources for shorter and longer workouts at varying intensities, but protein is critically important for many reasons beyond muscle growth, including :
- Muscle protein repair
- Bone health
- Remodeling protein in muscle, bone, tendons and ligaments
- To support a healthy immune system
- As a component of hormones, enzymes, and antibodies
- As a source of energy for the muscle, liver and intestines
- To maintain blood glucose (sugar) balance
- To increase lean body mass
- To produce plasma proteins
- To aid in weight management
Well, why do we have to eat enough protein everyday? We use the term protein balance. If the goals is to increase muscle mass, the key is to be in positive protein balance where protein synthesis is greater than protein breakdown. Even if one is not actively trying to increase muscle, muscle preservation is important and is influenced by protein sources, quantity and distribution over the day. And as we age, being preventive and proactive with exercise and protein intake may help to decrease the risk of sarcopenia- the muscle loss that occurs with aging.
Quality matters
Protein quality is determined by its amino acid composition and the body’s ability to breakdown and utilize those amino acids. For active individuals, consuming enough leucine is critically important as leucine can be the trigger for muscle protein synthesis. In addition, the dietary leucine requirement of older individuals may be higher than those of younger individuals. Szwiega S, Pencharz PB, Rafii M, Lebarron M, Chang J, Ball RO, Kong D, Xu L, Elango R, Courtney-Martin G. Dietary leucine requirement of older men and women is higher than current recommendations. Am J Clin Nutr. 2021 Feb 2;113(2):410-419. doi: 10.1093/ajcn/nqaa323. PMID: 33330915; PMCID: PMC7851820.
For those interested in increasing muscle mass, when soy protein is compared to whey protein , there are similar gains in muscle mass and strength when combined with resistance exercise. Messina M, Lynch H, Dickinson JM, Reed KE. No Difference Between the Effects of Supplementing With Soy Protein Versus Animal Protein on Gains in Muscle Mass and Strength in Response to Resistance Exercise. Int J Sport Nutr Exerc Metab. 2018 Nov 1;28(6):674-685. doi: 10.1123/ijsnem.2018-0071. Epub 2018 Oct 26. PMID: 29722584.
If the goal is to increase muscle mass, soy foods and soy protein supplements are appropriate choices for plant- based athletes as well as those who may not tolerate or are allergic to dairy foods and dairy based supplements.
So, if you eat primarily plant based protein , soy can be a great way to ensure you meet protein requirements through the foods you eat. And because it is so versatile, soy can be eaten alone or paired with other foods for nutrient amplification and flavorful combinations like these:
- A tofu/veggie stir fry
- Roasted edamame and popcorn trail mix
- Soy nut butter on bread
- Veggie crumbles and black bean taco with shredded cabbage and salsa
In addition, my athletes and clients are busy- between workouts, practices and jobs they don’t necessarily want to have to spend a lot of time in food preparation. Soy makes meal prep a breeze with taste to please. And of added bonus, soy on the plate contributes to plant intake and is often consumed with other fruits and vegetables such as a tofu stir fry, a soy yogurt and soy milk with fruit smoothie, or a tofu vegetable scramble. Soy delivers on portable , packable and non- perishable protein, such as roasted soy nuts, soynut butter and aseptic packages of soymilk so you can be on the go with your pro.
Protein Quantitiy
So how much protein do you need to eat everyday? The Recommended Dietary Allowances guidelines are for 0.4 grams of protein per pound body weight. Robert R Wolfe, Amy M Cifelli, Georgia Kostas, Il-Young Kim, Optimizing Protein Intake in Adults: Interpretation and Application of the Recommended Dietary Allowance Compared with the Acceptable Macronutrient Distribution Range, Advances in Nutrition, Volume 8, Issue 2, March 2017, Pages 266–275, https://doi.org/10.3945/an.116.013821
For a 150 pound individual, that would be about 54 grams of protein a day. So, is that enough? It depends upon your health, your activity level, and your weight goals. Protein is critically important to maintenance of lean mass especially when trying to lose body fat, but more than you need is just excess. Remember, when you are adding up your intake include the protein from supplements not just food.
If you are an athlete, exercising more than an hour daily, and you are trying to increase muscle, lose body fat, or prevent muscle loss, your protein needs may be higher. Also, older individuals who are active may have higher protein requirements than their sedentary counterparts for muscle preservation. Phillips SM, Van Loon LJ. Dietary protein for athletes: from requirements to optimum adaptation. J Sports Sci. 2011;29 Suppl 1:S29-38. doi: 10.1080/02640414.2011.619204. PMID: 22150425.
Jäger R, Kerksick CM, Campbell BI, Cribb PJ, Wells SD, Skwiat TM, Purpura M, Ziegenfuss TN, Ferrando AA, Arent SM, Smith-Ryan AE, Stout JR, Arciero PJ, Ormsbee MJ, Taylor LW, Wilborn CD, Kalman DS, Kreider RB, Willoughby DS, Hoffman JR, Krzykowski JL, Antonio J. International Society of Sports Nutrition Position Stand: protein and exercise. J Int Soc Sports Nutr. 2017 Jun 20;14:20. doi: 10.1186/s12970-017-0177-8. PMID: 28642676; PMCID: PMC5477153.
Protein Requirements
| Type of athlete |
Protein gms/lb BW |
150- pound individual |
| Recreational |
0.5-0.7 |
75-107 |
| Masters athletes |
0.54 |
81 |
| Endurance |
0.54-0.63 |
81-94 |
| Strength training |
0.72-0.77 |
108-115 |
| Teenage athlete |
0.7-0.9 |
105-135 |
| Gaining mass |
0.72-1.0 |
108-150 |
| Calorie restricted |
0.72 |
108 |
Protein distribution
When you consume protein is AS important as the amount consumed. Remember, the goal is to be in positive protein balance. So to do this, we must eat enough protein and include protein as part of every meal and snack. As a first step, think about how you consume protein. Do you eat very little protein-containing foods at breakfast and lunch and then a lot at dinner? If so, consider including protein-containing foods as part of each meal.
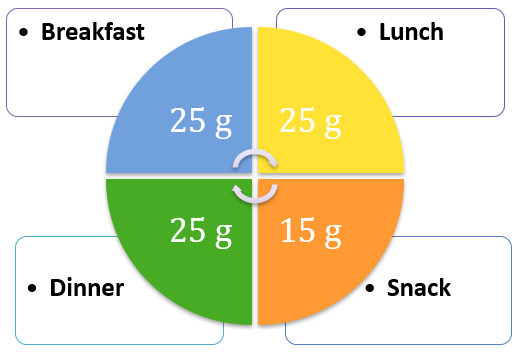
Protein timing for activity
I talk to my athletes and active clients about parenthesizing exercise with food. In other words, for more strenuous and/or longer duration activity, it is important to prefuel and re-fuel. The goal is to prepare for the activity –and repair from the activity you did so you can do it again. If your goal is to build muscle, the hand to mouth exercise is as important as the physical exercise. Carbohydrate and protein can be of benefit pre- and post- exercise, and a little goes a long way. Consuming smaller amounts pre- exercise can minimize gut distress. Ending exercise with a snack rather than a meal also works well.
Here are some suggestions:
- A soymilk smoothie
- Energy bites made with roasted soy nuts, soynut butter, oats, honey and dried fruit
- Soy yogurt with a little cereal
- A soy- based sports bar
Protein sources
So how do you know how much protein you are consuming?
If you are trying to have enough protein, aim for at least 20 -30 grams of protein at a meal. This can be a combination of animal and plant –based protein sources. Although 20-30 grams of protein per meal may not seem like much, we must also consider gut comfort, volume and amount of time allotted to eat between workouts, jobs, classes, etc. There are many plant based- proteins to choose from but they must fit within a calorie cap, gut comfort, time to consume, etc.
Soy foods are a quick prep, and provide a significant amount of protein in a small volume. Many are low in fat, to minimize gut discomfort, and can be consumed in several different forms. Some of my male athletes and active clients have expressed concern that eating soy foods could lower testosterone levels and increase estrogen. There is a misperception among some males, that the isoflavones or phytoestrogens in soy will alter hormone levels. Soy and soy isoflavones have no effect on testosterone or estrogen levels in men. Katharine E. Reed, Juliana Camargo, Jill Hamilton-Reeves, Mindy Kurzer, Mark Messina, Neither soy nor isoflavone intake affects male reproductive hormones: An expanded and updated meta-analysis of clinical studies ,Reproductive Toxicology.Volume 100,2021,https://doi.org/10.1016/j.reprotox.2020.12.019. (https://www.sciencedirect.com/science/article/pii/S0890623820302926)
From a culinary and versatility perspective, soy can be consumed as is, or dressed up with other foods, spices, sauces, etc. Here are some easy ways to incorporate soy into your day.
Breakfast
- Higher protein cereal or granola with soy milk , fruit and pistachios
- Soy based sausage breakfast sandwich
- Scrambled tofu with spinach and mushrooms and a side of potatoes
- Smoothie made with soy yogurt soy milk, fruit
Lunch
- Lentil soup with veggie crumbles, canned tomatoes and rice
- Flavored baked tofu on a salad with slivered almonds and mango
- Shelled edamame, rice noodles shredded carrots, pineapple in a soy sauce-peanut butter dressing
Snacks
- Hummus with soy protein isolate added served with veggies and pita chips
- Roasted edamame, dried fruit and cereal trail mix
- Soy yogurt with fruit and granola
Dinner
- Pasta with veggie crumbles in the sauce as well as pureed cannellini beans
- Stir fry with ginger teriyaki tofu, cashews, veggies over rice
- Grilled tofu or tempeh/veggie kebabs over soba noodles
Implementation
Keep a protein log to see how much protein you are consuming over the course of the day. To meet your protein needs, try to consume protein at each meal along with produce
(fruits/veggies) and some type of grain. Include protein at snacks as well as meals.
Bottom line
It’s important to get it right with your protein bites. Consuming high quality protein like soy as well as trying to more evenly distribute protein over the day rather than just focusing a daily number of grams of protein to consume can help you to be well, stay well and play well.

















